What is Syphilis?
Syphilis is a sexually transmitted disease. It is caused by the bacterium Treponema pallidum, and its most common symptom is a painless ulcer in the genital area.
If not properly treated, syphilis develops as a three-stage disease: primary, secondary, and tertiary syphilis. Each stage has different symptoms, and in the more advanced stages, the infection can spread throughout the body, causing severe damage to internal organs such as the heart and brain, and deforming lesions on the skin.
In the pre-antibiotic era, syphilis was a chronic, prolonged, painful, disfiguring disease that was extremely feared and highly stigmatized. Today, however, it is easily treated with antibiotics and cured at a high rate. Most cases are diagnosed at stage 1 or 2, and patients can be cured without major sequelae.
How T. pallidum gets transmitted
T. pallidum is primarily transmitted sexually. The bacteria enter the body through microscopic wounds or abrasions on the vaginal or penile mucosa.
The risk of transmission is estimated to be about 30% for each episode of unprotected sexual intercourse with an infected partner. If there are any sores or inflammation in the vagina or on the penis, the risk of infection is even higher.
Patients who transmit T. pallidum are those who have the disease in the primary or secondary stage, especially if there are active lesions in the genital organs.
Although not 100% effective, the condom is still the best method to prevent sexual transmission.
In the more advanced stages of the disease, the bacteria can be transmitted by kissing and even by touching the skin or mouth if there are active lesions, as will be discussed later.
At present, syphilis transmission by blood transfusion is very rare because Treponema pallidum does not survive for more than 48 hours under the current conditions in which blood is stored in blood banks.
There is also congenital syphilis, acquired by the fetus when the mother is infected with Treponema pallidum during pregnancy. Infection in pregnant women can cause miscarriage, premature birth, malformations, and fetal death.
Signs and Symptoms
As mentioned, Treponema pallidum infection has three stages, called primary, secondary, and tertiary syphilis.
Symptoms of primary syphilis
The incubation period, the time between infection and the onset of symptoms, averages 2 to 3 weeks. But in some cases, this period can be as short as three days or as long as three months.
The primary lesion of syphilis is a papule (a small elevation on the skin) on the genitals. Within a few hours, the papule turns into an ulcer, which is usually painless. This lesion may go unnoticed in women because it is small, on average 1 cm (0.4 in) in diameter, painless, and usually hidden between the pubic hair or inside the vagina.
The syphilis ulcer is called a chancre. After 3 to 6 weeks, the lesion will disappear even if no treatment is given, leading to the false impression of spontaneous healing. There are no other symptoms associated with the primary lesion. Apart from the chancre, the patient may, at most, experience enlargement of the inguinal lymph nodes.
In some cases, the ulcer may appear in the mouth or throat if transmission has occurred through oral sex.
Therefore, syphilis is initially a painless disease that usually goes unnoticed and disappears spontaneously after a while. That is the major issue. Any treatment, no matter how ineffective, can give the impression that it is effective because the chancre will disappear one way or another. This disappearance, however, does not mean that it has been cured. On the contrary, the bacteria may be multiplying and spreading silently throughout the body.
Symptoms of Secondary Syphilis
In 25% of untreated patients in the primary stage, syphilis returns after a few weeks or months. At this point, the disease has spread throughout the entire body.
Patients often remain unaware of their infection until the secondary stage, as the initial lesion may have been easily overlooked.
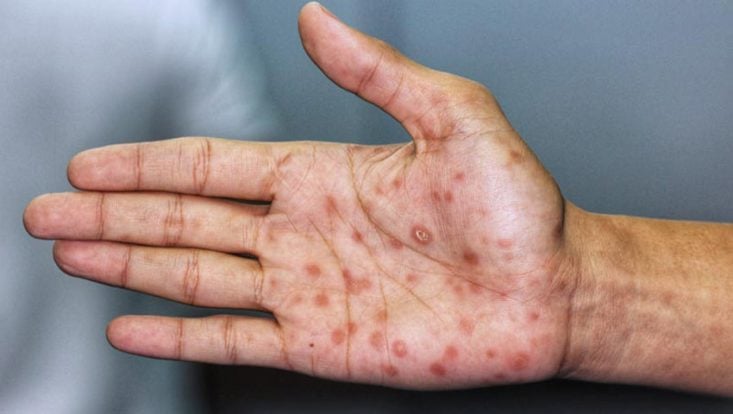
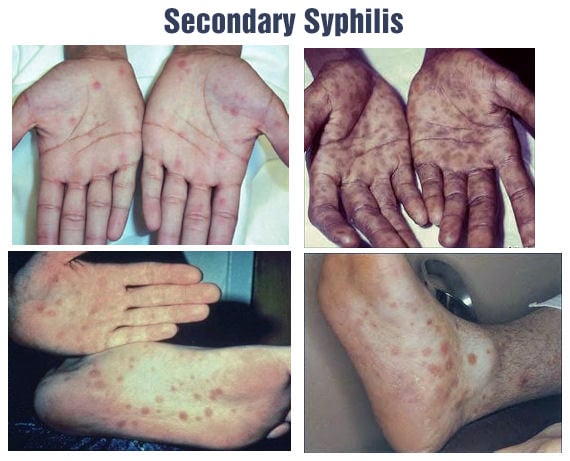
Secondary syphilis manifests with skin rashes, classically on the palms and soles. Other common symptoms include fever, malaise, loss of appetite, joint pain, hair loss, eye lesions, and enlargement of lymph nodes diffusely throughout the body.
The most characteristic manifestation is lesions on the soles, palms, and oral mucosa, but rashes can occur anywhere.
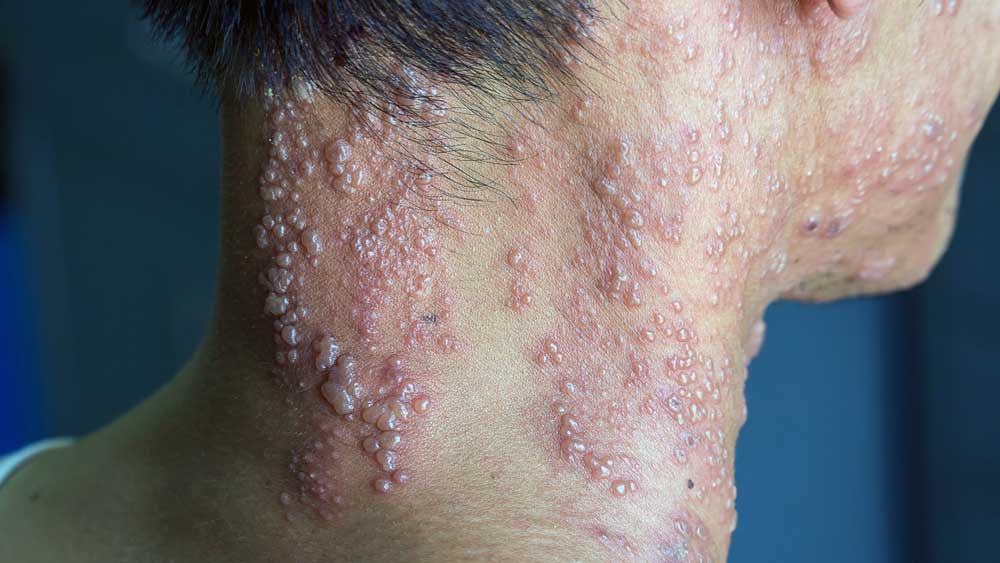
Another typical lesion of secondary syphilis is the so-called condyloma lata, a moist lesion with the appearance of a large wart, which usually appears close to the site of the chancre in the primary stage.
However, there are cases in which secondary syphilis has few symptoms, and the patient is unaware of the condition. About 20% of patients in the secondary stage do not find their symptoms bothersome enough to seek medical help.
As in the primary stage, the symptoms of secondary syphilis disappear spontaneously without treatment.
Latent syphilis
After the lesions in the secondary stage disappear, the patient enters the latent stage of the disease. There are no symptoms, but laboratory tests for syphilis remain positive (I will discuss this later).
The latent syphilis is divided into early latent syphilis, when the Treponema pallidum infection occurred less than one year ago, and late latent syphilis, when the infection occurred more than one year ago.
If we do not know when the patient was infected, it is assumed that the patient is in the late latent phase.
Patients in the early latent stage can infect their partners if they have unprotected sex. Patients in the late latent stage are usually no longer contagious.
Pregnant women with latent syphilis can transmit T. pallidum to the fetus if infected less than 4 years ago.
Symptoms of tertiary syphilis
Patients may remain asymptomatic in the latent phase for several years, even decades, before the disease returns. This new phase, when symptoms return, is called tertiary syphilis, the most severe form of the disease.
The tertiary phase presents three types of manifestations:
- Gummatous syphilis: large ulcerated lesions that can affect the skin, bones, and internal organs.
- Cardiovascular syphilis: involvement of the aorta, causing aneurysms and lesions of the aortic valve (see: What is an aneurysm?).
- Neurosyphilis: affects the nervous system, leading to dementia, meningitis, strokes, and motor problems due to damage to the spinal cord and nerves.
Currently, many authors divide syphilis into only two phases: early syphilis and late syphilis. Early syphilis includes all stages within the first year of infection, such as primary, secondary, and early latent syphilis. Late syphilis includes the late latent syphilis and tertiary syphilis. This division helps guide the treatment regimen (more on this later).
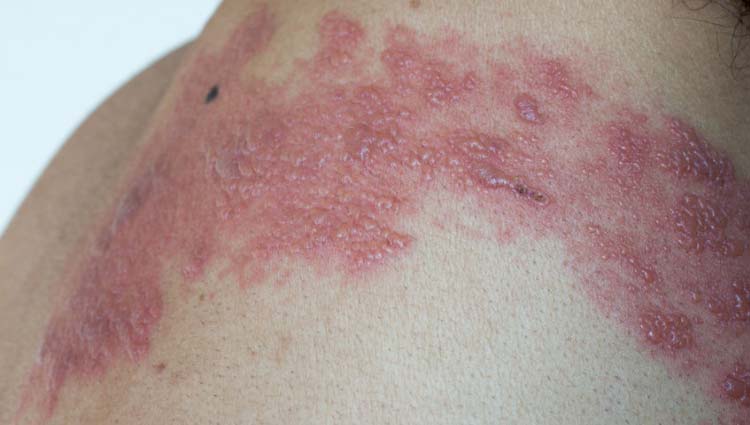
To see actual images of syphilis lesions in their different stages, click on the link: Pictures: Syphilis – All stages [Warning: Strong Images].
Serologic Diagnosis
In primary syphilis, when the chancre appears, the body may not have had time to produce antibodies against Treponema pallidum, so blood tests may be negative at this stage (about 20 to 30% of cases).
Laboratory confirmation can be done after taking material from the ulcer for direct visualization of the bacteria under a microscope. This test is not always necessary because the genital ulcer is very characteristic. Usually, the doctor starts treatment based on clinical data only, waiting one or two weeks to confirm the diagnosis in the laboratory if the first test is negative.
The diagnosis of syphilis is typically made by two serologic tests: nontreponemal tests, such as VDRL or RPR, and treponemal tests, such as FTA-ABS or TPHA.
Nontreponemal tests
There are three nontreponemal tests:
- Rapid plasma reagin (RPR).
- Venereal Disease Research Laboratory (VDRL).
- Toluidine Red Unheated Serum Test (TRUST).
The VDRL is the most widely used of these three in clinical practice.
These tests are called nontreponemal because they detect antibodies not to the Treponema pallidum bacterium itself, but to a combination of antigens called cardiolipin, cholesterol, and lecithin that are also present in patients infected with syphilis.
Although the test is cheaper and easier for laboratories to perform, because it does not directly test for Treponema pallidum antibodies, there is a higher risk of false-positive results.
As mentioned above, the VDRL is the simplest and most widely used screening test for syphilis. Its result is given in dilution form, i.e., a 1/8 (1:8) result means that the antibody has been identified up to 8 dilutions; a 1/64 result indicates that we can detect antibodies even after diluting the blood 64 times.
The higher the dilution at which the antibody can still be detected, the more positive the result. If you thought the explanation was confusing, know that the VDRL of 1/2 is a lower titer than 1/4, which is lower than 1/8, and so on. The higher the titer, the more positive the test.
The VDRL usually becomes positive between 2 and 6 weeks after contamination. In general, its values begin to rise significantly one to two weeks after the appearance of the chancre. Therefore, if the test is performed early, one or two days after the appearance of the ulcer, the result may be false negative.
VDRL levels are used to monitor the effectiveness of treatment, as they typically decrease after the infection has been cured (we will explain cure criteria later).
False-Positive VDRL
VDRL may be falsely positive in 1 to 2% of the population. False-positive cases usually occur in patients with the following characteristics or diseases:
- Individuals older than 70 years of age.
- Injecting drug users.
- Lupus.
- Liver diseases.
- Mononucleosis.
- Hansen’s disease (leprosy).
- Chicken Pox.
- Rheumatoid Arthritis.
- Rickettsial infection.
- Infective endocarditis.
- HIV infection.
In general, false-positive results have titers below 1/8, but titers as high as 1/256 have been described in patients without syphilis.
It is important to note that although infected patients usually have titers above 1/16, it is quite possible for an infected patient to have low VDRL titers. Therefore, any positive result should be confirmed with a treponemal test.
Treponemal Tests
The treponemal tests look directly for antibodies to the Treponema pallidum bacteria. Although they are more specific, they are more complex to perform, so they are frequently not the first choice for screening.
There are five treponemal tests:
- Fluorescent treponemal antibody absorption (FTA-ABS).
- Microhemagglutination test for antibodies to T. pallidum (MHA-TP).
- T. pallidum particle agglutination test (TPPA).
- T. pallidum enzyme immunoassay (TP-EIA).
- Chemiluminescence Immunoassay (CIA).
FTA-ABS is still the most widely used treponemal test, although TP-EIA has recently gained popularity. Its immunologic window is shorter, it can be positive a few days after the appearance of the chancre, and its false positive rate is lower than that of VDRL.
Unlike VDRL, which declines progressively with healing and may become negative after a few years, once positive, FTA-ABS remains so even after the patient is cured. However, some people treated for primary syphilis may become FTA-ABS negative after two or three years.
Usually, VDRL is used to screen for the disease and FTA-ABS for confirmation if the first test is positive. A diagnosis of syphilis should not be made with only one of these tests.
Interpretation of Serologic Testing
When investigating a possible case of syphilis, the following situations may occur:
- VDRL positive and FTA-ABS positive: both positive tests confirm the diagnosis.
- Positive VDRL and negative FTA-ABS: a different treponemal test must be performed to confirm the result. A new negative result indicates a disease other than syphilis. Reasons for false-positive VDRL should be investigated.
- Negative VDRL and positive FTA-ABS: this result can occur in three situations: very early infection, cured disease, or tertiary syphilis.
- Negative VDRL and negative FTA-ABS: both negative tests exclude the diagnosis of syphilis (there are rare cases when the test is done too early, and false negatives can occur in both).
Syphilis Treatment
Treatment for syphilis varies depending on the stage of the disease. The most recommended regimens are:
- Early syphilis (primary, secondary, or early latent syphilis): penicillin G benzathine 2.4 million units single dose.
- Late syphilis (syphilis with more than 1 year of evolution, tertiary or of undetermined time): penicillin G benzathine 2.4 million units in 3 doses, one week apart, totaling 7.2 million units.
Cases involving the neurological system (neurosyphilis) should not be treated with penicillin G benzathine, but with IV penicillin G (3 to 4 million units IV every four hours) for 10 to 14 days.
Treatment should always be with penicillin, including in pregnant and breastfeeding women.
In some cases, such as infection in pregnant women, treatment to desensitize the allergic patient to penicillin may be indicated.
Other antibiotics should only be used if the patient is allergic to penicillin and is unwilling or unable to undergo desensitization.
Patients with penicillin allergy may be treated with doxycycline (100 mg twice daily for 14 days). If the patient is allergic to penicillin but not to cephalosporins, an option is ceftriaxone (1 g daily intramuscularly for 14 days). Both regimens are less effective than benzathine penicillin.
Azithromycin (single dose of 2 grams) was once indicated as an alternative to penicillin, but is now considered a less effective option.
Jarisch-Herxheimer Reaction
The Jarisch-Herxheimer reaction is an acute, self-limited, febrile reaction that usually occurs within the first 24 hours after a patient begins treatment for syphilis. This reaction occurs in approximately 10-35% of cases of primary, secondary, or early latent syphilis.
The fever may be accompanied by other symptoms such as headache, muscle aches, heavy sweating, low blood pressure, and worsening of the rash, if present initially.
There is no way to avoid this reaction. Patients should be informed of possible signs and symptoms and advised to contact their physician if a severe reaction occurs.
Although symptoms usually resolve spontaneously within 12 to 24 hours, non-steroidal anti-inflammatory drugs (NSAIDs) or other antipyretics, such as acetaminophen or dipyrone, may be used to reduce the severity of symptoms and the duration of the reaction.
Is syphilis curable?
Yes, syphilis is curable if treated with appropriate antibiotics, preferably penicillin G benzathine at the doses indicated above. With proper treatment, the cure rate is greater than 95%.
After starting treatment, the lesions begin to disappear in the first few days. However, it is necessary to repeat the blood tests to confirm the cure.
Cure criteria
Each treated patient must repeat the VDRL after 6 and 12 months. The cure criteria for syphilis are the disappearance of symptoms and a fourfold decline in the nontreponemal titer (two dilutions decrease). Examples:
- VDRL was 1/64 and dropped to 1/16 after treatment.
- VDRL was 1/32 and dropped to 1/8 after treatment.
- VDRL was 1/128 and dropped to 1/32 after treatment.
As time passes, titers will continue to decline and may even become negative after a few years (there are cured patients who remain lifelong with low titers, such as 1/2 or 1/4). The VDRL doesn’t need to be negative to certify that syphilis has been cured.
Primary syphilis titers decline more rapidly than secondary and tertiary stages. The FTA-ABS is not useful for treatment monitoring because, as explained above, it usually does not become negative after the cure. Once positive, the FTA-ABS may remain positive for the rest of your life. This is called immunological scarring.
References
- Syphilis – Harrison’s Principles of Internal Medicine 19th ed.
- Syphilis infection – BMJ BestPractice.
- Sexually transmitted diseases treatment guidelines, 2015 – Centers for Disease Control and Prevention.
- 2014 European Guideline on the Management of Syphilis – The International Union against Sexually Transmitted Infections (IUSTI).
- Syphilis Detection Test – Medscape.
- Syphilis: Epidemiology, pathophysiology, and clinical manifestations in HIV-uninfected patients – UpToDate.
- Syphilis: Treatment and monitoring – UpToDate.
- Syphilis: Screening and diagnostic testing – UpToDate.
- Syphilis – World Health Organization.
Author(s)
Pedro Pinheiro holds a medical degree from the Federal University of Rio de Janeiro (UFRJ) and is a specialist in Internal Medicine and Nephrology, certified by the State University of Rio de Janeiro (UERJ) and the Brazilian Society of Nephrology (SBN). He is currently based in Lisbon, Portugal, with his credentials recognized by the University of Porto and the Portuguese Nephrology Specialty College.






![Pictures: Syphilis – All stages [Warning: Strong Images]](https://www.mdsaude.com/wp-content/uploads/sifilis-imagem.jpg)
Leave a Comment