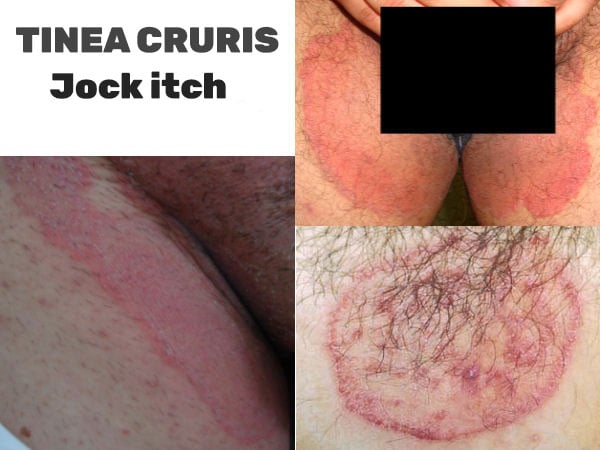
What is Jock Itch?
Jock itch, also known as tinea cruris or groin ringworm, is a common fungal infection. It belongs to a group of fungal skin infections called tinea or dermatophytosis, which are caused by fungi of the genera Trichophyton, Microsporum, or Epidermophyton.
Dermatophytoses can affect different areas of the body, such as the scalp (tinea capitis), feet (tinea pedis), beard (tinea barbae), nails (tinea unguium), or trunk and limbs (tinea corporis).
The fungal infection that affects the genital area, thighs, buttocks, and groin is called tinea cruris. Tinea cruris is the second most common dermatophytosis after tinea pedis, which is a fungal infection of the feet, popularly known as athlete’s foot.
Tinea cruris is usually a mild and harmless infection. Still, it can spread quickly to surrounding areas if it develops in warm and moist places, such as the folds of the thighs and buttocks.
Tinea cruris is more common in men and adolescent boys and causes reddened skin lesions that are very itchy.
Causes
The vast majority of cases of groin ringworm are caused by the fungus Trichophyton rubrum. This fungus can be a normal inhabitant of the skin without necessarily causing disease because our immune system can keep it under control as long as the skin is kept clean and dry. In warmer weather, however, some areas of the body, such as the groin and genital area, are constantly moist and hot, which favors the proliferation of fungi, resulting in a fungal infection.
The fungus that causes jock itch, Trichophyton rubrum, is the same fungus that causes athlete’s foot. Therefore, in many cases, the patient has dermatophytosis of the feet and groin simultaneously.
Transmission
Tinea cruris is a contagious infection transmitted by fomites, such as towels, sheets, or clothing contaminated with the fungus.
Tinea cruris can also occur as self-contamination from fungal infections of the feet (athlete’s foot). After touching the feet, the patient’s hands may come into contact with the fungus, which can then be transferred to the groin area. Sexual contact with an infected person can also spread the infection.
Risk Factors
However, in order to develop ringworm, it is not enough to simply come into contact with the fungus. The microorganism needs to find a favorable environment in which to multiply and overcome our immune system. Heat, moisture, and lack of light are the most favorable conditions for fungal growth.
The groin is very susceptible to fungal infections because it is not only covered for much of the day, but it is an area of folds and hair that is often damp and warm.
Hot weather, wearing hot, tight clothing, excessive sweating, staying in wet swimsuits for too long, poor personal hygiene, and not changing underwear frequently are all factors that promote the development of tinea cruris.
Some additional factors that can increase the risk of developing ringworm in the groin area are:
- Male gender (tinea cruris is three times more common in men).
- Hyperhidrosis.
- Participation in high-impact contact sports, such as wrestling.
- Obesity.
- Diabetes mellitus.
- HIV infection.
- Psoriasis.
- Atopic dermatitis.
Skin mycoses are more common in people with weakened immune systems, but they are also common in healthy people without health problems.
Symptoms
The main symptoms of jock itch are itching and localized redness. The inflamed area may be stinging, making it uncomfortable to wear certain types of underwear.
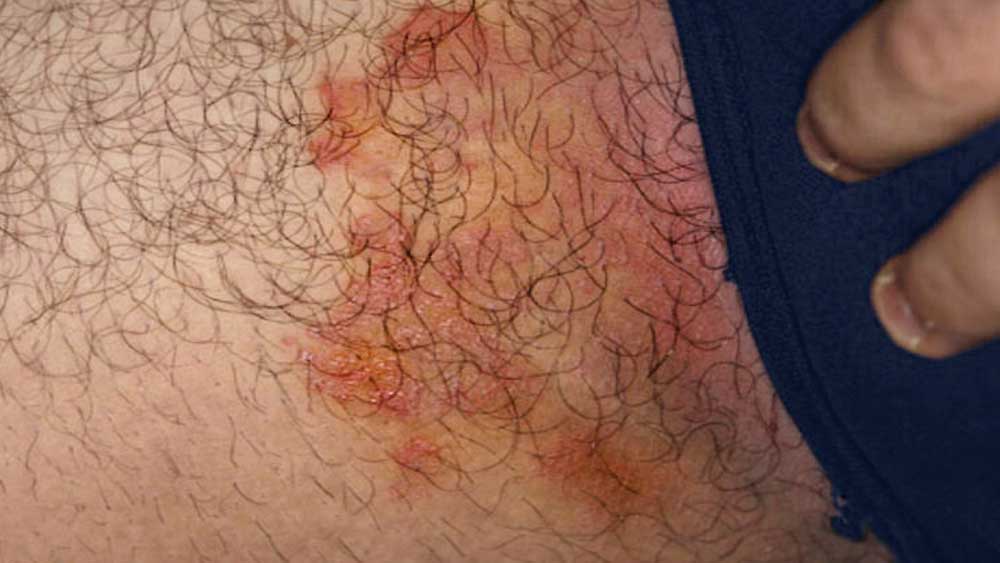
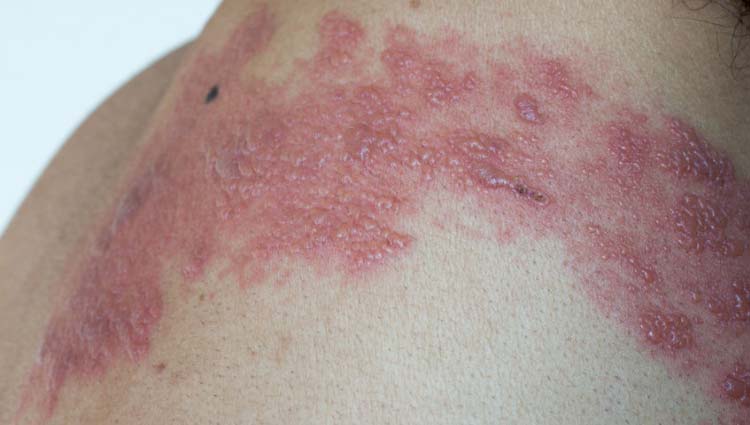
Tinea cruris usually starts as a reddish plaque on the inside of one or both thighs, with well-demarcated borders. When caused by the fungus Trichophyton rubrum, the disease usually extends downward, across the thighs, and even into the pubic area and buttocks. The lesions are typically circular in shape.
In half of the cases, the patient also has another type of tinea, usually tinea pedis (jock itch).
In men, the scrotum and penis are usually spared. This is an important feature as it helps to distinguish tinea cruris from a Candida infection, as Candidiasis of the inguinal region in men often involves the scrotum.
The diagnosis can be confirmed by scraping the lesion and microscopic examination of the material for fungi. Because Candida and dermatophytes are fungi with different characteristics, they can be distinguished by microscopic examination.
For more pictures of typical tinea cruris lesions, click the following link: Photos of tinea cruris.
Treatment
Groin ringworm can be treated with antifungal ointments, many of which are available over-the-counter. Treatment should be carried out for 2 to 4 weeks.
There are several options for topical treatment of jock itch with creams or ointments. The most suitable for tinea cruris are those containing one of the following antifungals:
- Ketoconazole: 2% cream, apply once a day.
- Miconazole: 2% cream, applied twice a day.
- Tioconazole: 1% cream, apply twice a day.
- Clotrimazole: 1% cream, apply twice a day.
- Oxiconazole: 1% cream, apply 1-2 times a day.
- Ciclopirox: 0.77% cream, apply twice a day.
- Butenafine: 1% cream, apply once a day.
- Naphthyfine: 1 or 2% cream, apply once a day.
- Terbinafine: 1% cream, apply 1 to 2 times a day.
- Tolnaftate: 1% cream, apply twice a day.
The first six substances on the list act against dermatophytes and Candida. The last four treat dermatophytosis, but are less effective against Candida.
Creams or ointments based on nystatin work for candidiasis but not for dermatophytosis, and are not indicated for the treatment of tinea cruris.
Ointments containing corticosteroids, such as betamethasone or triamcinolone, should be avoided as these substances may interfere with treatment and mask symptoms.
In immunosuppressed patients or when ointments don’t work, oral medications, such as griseofulvin, fluconazole, or terbinafine, may be prescribed.
Because tinea pedis (athlete’s foot) and onychomycosis (nail fungus) are risk factors for tinea cruris, it is important to treat both conditions to reduce the risk of recurrence of jock itch.
Applying talcum powder to the groin daily helps keep the area dry and prevent recurrences.
Patients should be advised to avoid hot baths and tight clothing. Men should wear loose-fitting underwear, preferably boxer shorts. Women should wear cotton briefs and avoid tight pants.
After showering, the groin area should be dried thoroughly. It is advisable to use one towel to dry the infected area and another towel for the rest of the body. Do not wear the same underwear after bathing.
REFERences
- Dermatophyte (tinea) infections – UpToDate.
- Diagnosis and Management of Tinea Infections – American Family Physician.
- Topical antifungal treatments for tinea cruris and tinea corporis – The Cochrane database of systematic reviews.
- Tinea Cruris – Medscape.
Author(s)
Pedro Pinheiro holds a medical degree from the Federal University of Rio de Janeiro (UFRJ) and is a specialist in Internal Medicine and Nephrology, certified by the State University of Rio de Janeiro (UERJ) and the Brazilian Society of Nephrology (SBN). He is currently based in Lisbon, Portugal, with his credentials recognized by the University of Porto and the Portuguese Nephrology Specialty College.







Leave a Comment